Diabetes-Related Nerve Sensations: Early Neuropathy Warning Signs
by Maroa Noa · 07 Apr 2026
Diabetes can affect far more than blood sugar levels alone. Over time, persistently high blood glucose may damage the nerves, leading to unusual sensations that many people dismiss in the early stages.
Tingling feet, burning pain, numbness, or a crawling sensation under the skin may seem minor at first, but these can be among the earliest warning signs of diabetic neuropathy.
Many people live with diabetes for years before recognizing that changes in their feet, hands, or legs may signal nerve damage.
The earlier you identify these symptoms, the greater your chance of slowing progression through better glucose control, medical support, and protective self-care.
In Kenya, where diabetes is becoming increasingly common, awareness of early neuropathy warning signs is essential for preventing long-term complications.
This article explains what diabetic neuropathy is, the early warning signs to watch for, risk factors, treatment approaches, lifestyle measures, and helpful products that may support symptom management.
What Is Diabetic Neuropathy?
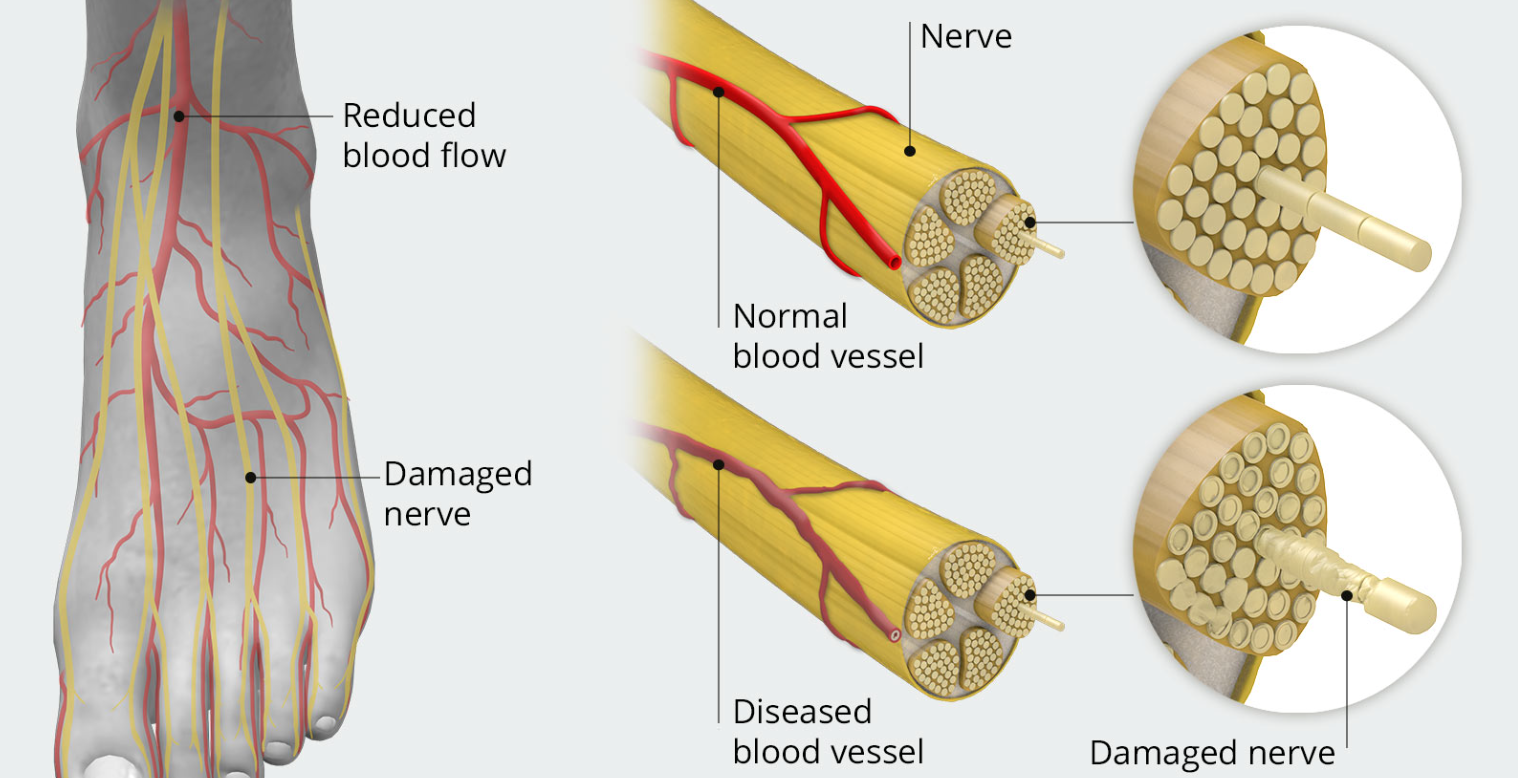
Diabetic neuropathy is a form of nerve damage caused by prolonged high blood sugar levels. Excess glucose can injure the small blood vessels that supply the nerves, reducing oxygen and nutrients to the nerve tissue.
Over time, this condition interferes with the way nerves send signals, causing pain, numbness, weakness, or abnormal sensations.
Although diabetic neuropathy can affect different parts of the body, the most common type is peripheral neuropathy, which usually begins in the feet and legs before sometimes affecting the hands.
This is why many people first notice symptoms such as tingling toes, burning feet, or reduced sensitivity when walking.
Diabetic neuropathy does not always begin with severe pain. Often, the earliest signs are subtle and intermittent, which makes them easy to ignore until the damage becomes more advanced.
Why Early Detection Matters
Early recognition of nerve symptoms can make a major difference. When neuropathy is identified in its early stages, blood sugar management, foot care, and medical treatment may help reduce symptom severity and slow further nerve damage.
Ignoring nerve changes can lead to more serious complications. Reduced sensation in the feet increases the risk of unnoticed injuries, ulcers, infections, and delayed healing.
This is particularly concerning for people with diabetes because even small cuts or blisters can become serious if circulation is poor or infections develop.
Early action is therefore not just about comfort. It is also about protecting mobility, independence, and long-term quality of life.
Early Neuropathy Warning Signs to Watch For
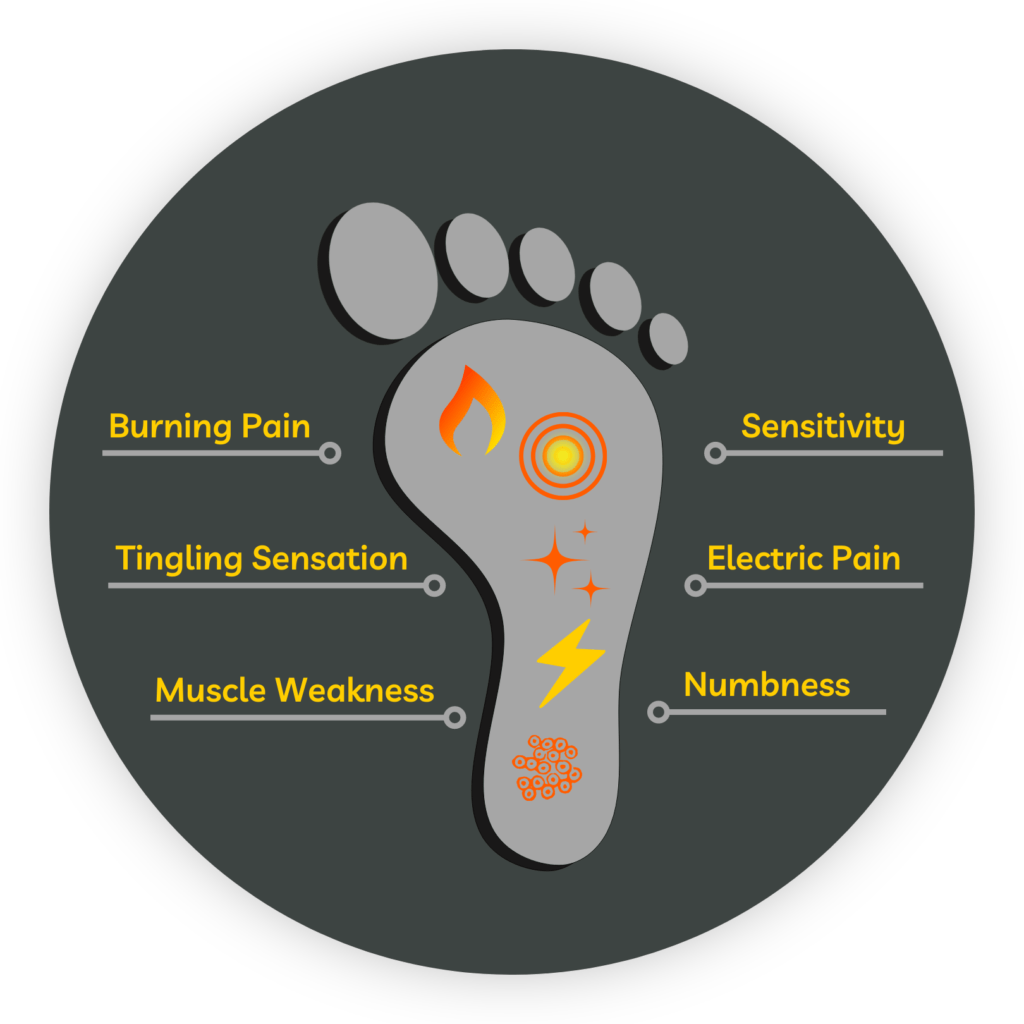
The first signs of diabetic neuropathy often develop gradually. They may come and go, especially at night, and may affect both feet symmetrically.
Tingling or “Pins and Needles”
A tingling sensation in the toes or soles of the feet is one of the most common early symptoms. Some people describe it as prickling, buzzing, or feeling like tiny electric pulses under the skin.
Burning Sensations
Burning feet, especially at night, are a classic sign of developing nerve irritation. The discomfort may range from mild warmth to intense burning pain that interferes with sleep.
Numbness or Reduced Sensation
Some people notice the opposite of pain. Instead of burning or tingling, they may begin to lose feeling in their toes or feet. This condition can make it difficult to detect injury, pressure, heat, or cold, increasing the risk of unnoticed wounds.
Sharp, Stabbing, or Electric-Like Pain
Neuropathic pain may feel sudden, shooting, or electric. It can occur without any obvious injury and may worsen during periods of poor glucose control. These sensations can affect concentration, rest, and daily function.
Heightened Sensitivity to Touch
In some cases, the nerves become overreactive rather than numb. Light touch, socks, or bed covers may trigger discomfort. This abnormal sensitivity can be just as distressing as numbness.
Muscle Weakness or Unsteadiness
As nerve damage progresses, some people notice weakness, poor balance, or difficulty walking steadily. This may increase the risk of falls and reduce confidence in daily movement.
Common Risk Factors for Diabetic Neuropathy
Not everyone with diabetes develops neuropathy at the same rate. Several factors increase the risk.
Poorly controlled blood sugar is the most important contributor. The longer blood glucose remains above target, the greater the chance of nerve injury. Duration of diabetes also matters, since nerve damage becomes more likely over time.
Other risk factors include high blood pressure, high cholesterol, smoking, obesity, alcohol misuse, and kidney disease.
These factors can impair blood flow and worsen nerve health. People with both diabetes and poor circulation are especially vulnerable to foot complications.
Why the Feet Are Often Affected First
The nerves that travel to the feet are among the longest in the body. Longer nerves are more vulnerable to damage from reduced blood supply and metabolic stress. This is why neuropathy often starts in the toes and gradually moves upward in a “stocking” pattern.
Because the feet bear weight every day, loss of sensation there is particularly dangerous. A person may continue walking on a blister, pressure point, or small cut without realizing it. Over time, this condition can lead to ulcers and infections that are difficult to treat.
How Diabetic Neuropathy Is Diagnosed
Diagnosis begins with a medical history and a review of symptoms. A healthcare professional may ask when the sensations started, where they occur, whether they worsen at night, and how diabetes has been managed.
A physical exam usually includes checking reflexes, balance, vibration sense, temperature sensation, and response to light touch.
In some cases, additional tests may be used to confirm nerve damage or rule out other causes such as vitamin deficiencies, thyroid disease, or medication side effects.
Treatment and Symptom Management
There is no single cure for diabetic neuropathy, but many people improve when the condition is managed early and consistently.
Better Blood Sugar Control
The foundation of treatment is improving glucose management. Stable blood sugar helps protect the nerves from further damage and may reduce symptom intensity over time. This often involves medication adherence, regular monitoring, meal planning, and physical activity.
Pain Relief and Prescription Support
Doctors may recommend medications specifically used for nerve pain. These are different from ordinary painkillers and may be more effective for burning, tingling, or shooting pain. Treatment should always be individualized.
Foot Care and Protection
Daily foot care is essential. Inspecting the feet daily, wearing comfortable footwear, avoiding barefoot walking, and treating small injuries promptly can help prevent complications. Moisturizing dry skin helps reduce cracks, but cream should not be applied between the toes unless advised.
Nutritional and Lifestyle Support
Good nutrition supports overall nerve health. Balanced meals, smoking cessation, reduced alcohol use, hydration, and regular physical activity can all contribute to better outcomes. Some people may also be evaluated for nutrient deficiencies, such as vitamin B12, especially if they take long-term metformin.
Products That May Help Support Management
1. On Call Plus Blood Glucose Meter - Regular glucose monitoring is one of the most important ways to reduce the risk of diabetic nerve damage, because persistently high blood sugar is a major driver of neuropathy progression.
2. Accu-Chek Instant Simple Meter 1’s - This is another Pharmily-listed glucose meter designed for fast, accurate home testing. Pharmily notes that it has a simple interface and a target range indicator, which can make it easier for people to understand whether a reading is within the goal.
3. Contour TS x 50 Strips - Test strips are essential if you are already using a compatible glucose meter and need consistent monitoring. Pharmily describes these strips as fast, accurate, and designed for the Contour TS meter, with no coding technology to reduce user error.
4. HealthAid Vitamin B12 Tablets 1000mcg 50s - Vitamin B12 is important for healthy nerve function, and Pharmily specifically states that this supplement helps maintain healthy nerve function and supports metabolism. This information can be especially relevant for people with diabetes who may have low B12, including some long-term metformin users.
5. Nature’s Aid Vitamin B12 1000mcg Sublingual Vegan 90’s - This Pharmily-listed B12 option is marketed for energy levels and nervous system health, with a sublingual format that some people find convenient. Sublingual tablets can be useful for users who prefer not to swallow standard tablets.
6. REGEN-D 150 Gel 15g - If neuropathy has already contributed to poor wound healing or to the risk of diabetic foot ulcers, this gel may be relevant. Pharmily states that it is clinically backed for use in diabetic foot ulcers and chronic wounds and supports skin regeneration.
When to See a Healthcare Professional
Seek medical advice if you have diabetes and notice recurring tingling, burning, numbness, unusual sensitivity, foot pain, or weakness. Prompt evaluation is especially important if symptoms disturb sleep, affect walking, or continue worsening.
Urgent care is needed if you develop foot ulcers, cuts that are not healing, swelling, signs of infection, blackened skin, or sudden, severe pain. These may indicate more serious complications requiring immediate treatment.
Final Thoughts
Diabetes-related nerve sensations are not symptoms to ignore. What starts as mild tingling or burning in the feet may be the earliest sign of diabetic neuropathy, a complication that can worsen silently if blood sugar and foot health are not managed carefully.
Recognizing early neuropathy warning signs gives you a better chance of protecting nerve function, preventing foot complications, and maintaining quality of life. In the Kenyan context, where diabetes awareness and early screening remain vital, learning these symptoms can support earlier intervention and better long-term outcomes.
Pay attention to the signals your body gives you. Early action, proper diabetes management, regular foot checks, and timely medical care can make a meaningful difference.
FAQs
1. What are the early signs of diabetic neuropathy?
Early signs include tingling, burning feet, numbness, sharp nerve pain, and unusual sensitivity to touch, especially in the toes and feet.
2. Can diabetic neuropathy happen even if diabetes seems mild?
Yes. Even people with recently diagnosed or moderately controlled diabetes can develop nerve symptoms, especially if blood sugar has been high for long periods without notice.
3. Is diabetic neuropathy reversible?
Some symptoms may improve with better blood sugar control and early treatment, but established nerve damage is often difficult to fully reverse. Early action offers the best chance of slowing progression.
4. Why is diabetic foot care so important?
Loss of sensation can prevent you from noticing injuries. Small wounds may worsen into ulcers or infections, so daily foot inspection is essential.
5. When should I see a doctor about nerve pain in diabetes?
You should seek medical advice if tingling, burning, numbness, weakness, or foot pain is recurring, worsening, or affecting sleep, walking, or balance